Paediatric Physiotherapy - Infant - Failure to Thrive (Orange)
Context of assessment: The student has been requested to perform a ward based, developmental assessment for a patient admitted to the ward for investigation of poor feeding and weight loss. It is expected that the patient will undergo a further developmental assessment at a later date, therefore, the student has been instructed to adequately assess the patient to acknowledge and reassure mother on possible developmental delay.
Background information for infant clinical scenario:
Setting: Acute inpatient paediatric ward
Gender: Female
Patient age: 6 months
Main Presentation: Failure to thrive, developmental delay
Student Name: Sally
Educator Name: Jenny
Patient/ Parent Name: Taylor and Cassie (mother)
Clinical History:
Reason for referral to physiotherapy:
Paediatricians have identified developmental delay
History of presenting condition:
Patient admitted to hospital via ED 4 days ago for investigation of failure to thrive (poor feeding, weight loss, dehydration and general irritability) and coffee ground vomiting. She is currently an inpatient on the paediatric ward of a hospital, receiving nasogastric feeds and awaiting endoscopy tomorrow for confirmation of suspected cow’s milk protein allergy and related oesinophilic oesophagitis.
Investigations:
Blood tests – elevated platelets
Stool sample – faecal leukocytes and positive for blood
Urine sample – (shows dehydration)
Growth chart – CW 4995g (less than 3rd centile)
Consulting teams
Paediatricians
Gastroenterology
Dietician
Social Worker
Past medical history:
Mum reports losing breast milk at 3 months and starting infant formula. Baby took formula initially and then started to become irritable, cry, looked in pain, periods of diarrhoea, intermittent cough and runny nose. Trialled different formulas with similar results. Took up to an hour for baby to take a bottle. Sometimes baby would refuse bottle. Had 2 GP visits. Sleeps poorly during day and wakes regularly through night. Recent onset of eczema on legs and arms. Has trialled Omeprazole (prescribed by GP) with no benefit.
Birth history
K39+0, BW 2954g (25th centile), SVD, APGARS 7,9,9
Normal pregnancy and scans
Passed healthy hearing newborn screen
Past surgical history:
Nil
Developmental history:
Smiling and cooing
Just starting to reach for toys
Never liked tummy time
Always has to be carried
Not rolling
Started on solids at 4 months
Medications:
Ranitidine (Zantac) – started in ED
Neocate infant formula – day 1 today
Social & Family History:
Mum (23yo) and Dad (24yo – Jack), married
First baby (G=1, P=1)
No local family support
Dad is a mechanic, Mum is on maternity leave from an office admin job.
Parents share a car and have good access to public transport
Parental concerns/goals:
Anxiety around baby’s health and the cause of this, current hospital admission and Doctor’s suggestion of developmental delay.
Видео Paediatric Physiotherapy - Infant - Failure to Thrive (Orange) канала Griffith Health
Background information for infant clinical scenario:
Setting: Acute inpatient paediatric ward
Gender: Female
Patient age: 6 months
Main Presentation: Failure to thrive, developmental delay
Student Name: Sally
Educator Name: Jenny
Patient/ Parent Name: Taylor and Cassie (mother)
Clinical History:
Reason for referral to physiotherapy:
Paediatricians have identified developmental delay
History of presenting condition:
Patient admitted to hospital via ED 4 days ago for investigation of failure to thrive (poor feeding, weight loss, dehydration and general irritability) and coffee ground vomiting. She is currently an inpatient on the paediatric ward of a hospital, receiving nasogastric feeds and awaiting endoscopy tomorrow for confirmation of suspected cow’s milk protein allergy and related oesinophilic oesophagitis.
Investigations:
Blood tests – elevated platelets
Stool sample – faecal leukocytes and positive for blood
Urine sample – (shows dehydration)
Growth chart – CW 4995g (less than 3rd centile)
Consulting teams
Paediatricians
Gastroenterology
Dietician
Social Worker
Past medical history:
Mum reports losing breast milk at 3 months and starting infant formula. Baby took formula initially and then started to become irritable, cry, looked in pain, periods of diarrhoea, intermittent cough and runny nose. Trialled different formulas with similar results. Took up to an hour for baby to take a bottle. Sometimes baby would refuse bottle. Had 2 GP visits. Sleeps poorly during day and wakes regularly through night. Recent onset of eczema on legs and arms. Has trialled Omeprazole (prescribed by GP) with no benefit.
Birth history
K39+0, BW 2954g (25th centile), SVD, APGARS 7,9,9
Normal pregnancy and scans
Passed healthy hearing newborn screen
Past surgical history:
Nil
Developmental history:
Smiling and cooing
Just starting to reach for toys
Never liked tummy time
Always has to be carried
Not rolling
Started on solids at 4 months
Medications:
Ranitidine (Zantac) – started in ED
Neocate infant formula – day 1 today
Social & Family History:
Mum (23yo) and Dad (24yo – Jack), married
First baby (G=1, P=1)
No local family support
Dad is a mechanic, Mum is on maternity leave from an office admin job.
Parents share a car and have good access to public transport
Parental concerns/goals:
Anxiety around baby’s health and the cause of this, current hospital admission and Doctor’s suggestion of developmental delay.
Видео Paediatric Physiotherapy - Infant - Failure to Thrive (Orange) канала Griffith Health
Показать
Комментарии отсутствуют
Информация о видео
Другие видео канала
 Developmental Milestones "Rolling From Back to Tummy Starts Around 5 to 7 Months" | KOTM.org
Developmental Milestones "Rolling From Back to Tummy Starts Around 5 to 7 Months" | KOTM.org How to do Clubfoot Stretches - Nemours KidsHealth
How to do Clubfoot Stretches - Nemours KidsHealth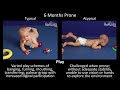 6 Month Old Baby Typical & Atypical Development Side by Side
6 Month Old Baby Typical & Atypical Development Side by Side 4 Month Old Baby Typical & Atypical Development Side by Side
4 Month Old Baby Typical & Atypical Development Side by Side Brachial Plexus Injury: Range of Motion Exercises
Brachial Plexus Injury: Range of Motion Exercises Teaching a Baby to Get into Sitting: Pediatric Physical Therapy #17
Teaching a Baby to Get into Sitting: Pediatric Physical Therapy #17 Welcome to Kids Physiotherapy
Welcome to Kids Physiotherapy Paediatric Physiotherapy - Infant - Failure to Thrive (Apple)
Paediatric Physiotherapy - Infant - Failure to Thrive (Apple) NECK CONTROL EXERCISES FOR CEREBRAL PALSY KIDS
NECK CONTROL EXERCISES FOR CEREBRAL PALSY KIDS Early Intervention For Kids with CP: Sonali Explores Neuroplasticity
Early Intervention For Kids with CP: Sonali Explores Neuroplasticity Cerebral Palsy Treatment with Multi-Modal Therapy - Part 1 | Trishla Foundation
Cerebral Palsy Treatment with Multi-Modal Therapy - Part 1 | Trishla Foundation Passive Limb Exercise For 1-3 Month Old
Passive Limb Exercise For 1-3 Month Old Exercise to Improve Neck Holding & Trunk control in Cerebral Palsy Children | Trishla Foundation
Exercise to Improve Neck Holding & Trunk control in Cerebral Palsy Children | Trishla Foundation Paediatric Physiotherapy - Toddler - Developmental Coordination Disorder (Mango)
Paediatric Physiotherapy - Toddler - Developmental Coordination Disorder (Mango) Rolling Back to Side, Head Control: Pediatric PT Strengthening for Babies #6
Rolling Back to Side, Head Control: Pediatric PT Strengthening for Babies #6 physiotherapy exercises for cerebral palsy, occupational therapy delayed milestone, autism in hindi
physiotherapy exercises for cerebral palsy, occupational therapy delayed milestone, autism in hindi Head Control in Sitting: Exercises For a Baby with Low Tone #1
Head Control in Sitting: Exercises For a Baby with Low Tone #1 Paediatric Physiotherapy - Adolescent - Cerebral Palsy (Melon)
Paediatric Physiotherapy - Adolescent - Cerebral Palsy (Melon) "Chest Physiotherapy" by Susan Hamilton, MS, RN, for OPENPediatrics
"Chest Physiotherapy" by Susan Hamilton, MS, RN, for OPENPediatrics Cerebral Palsy @ Dr, Ajay Kumar, Child Neurologist in Patna
Cerebral Palsy @ Dr, Ajay Kumar, Child Neurologist in Patna